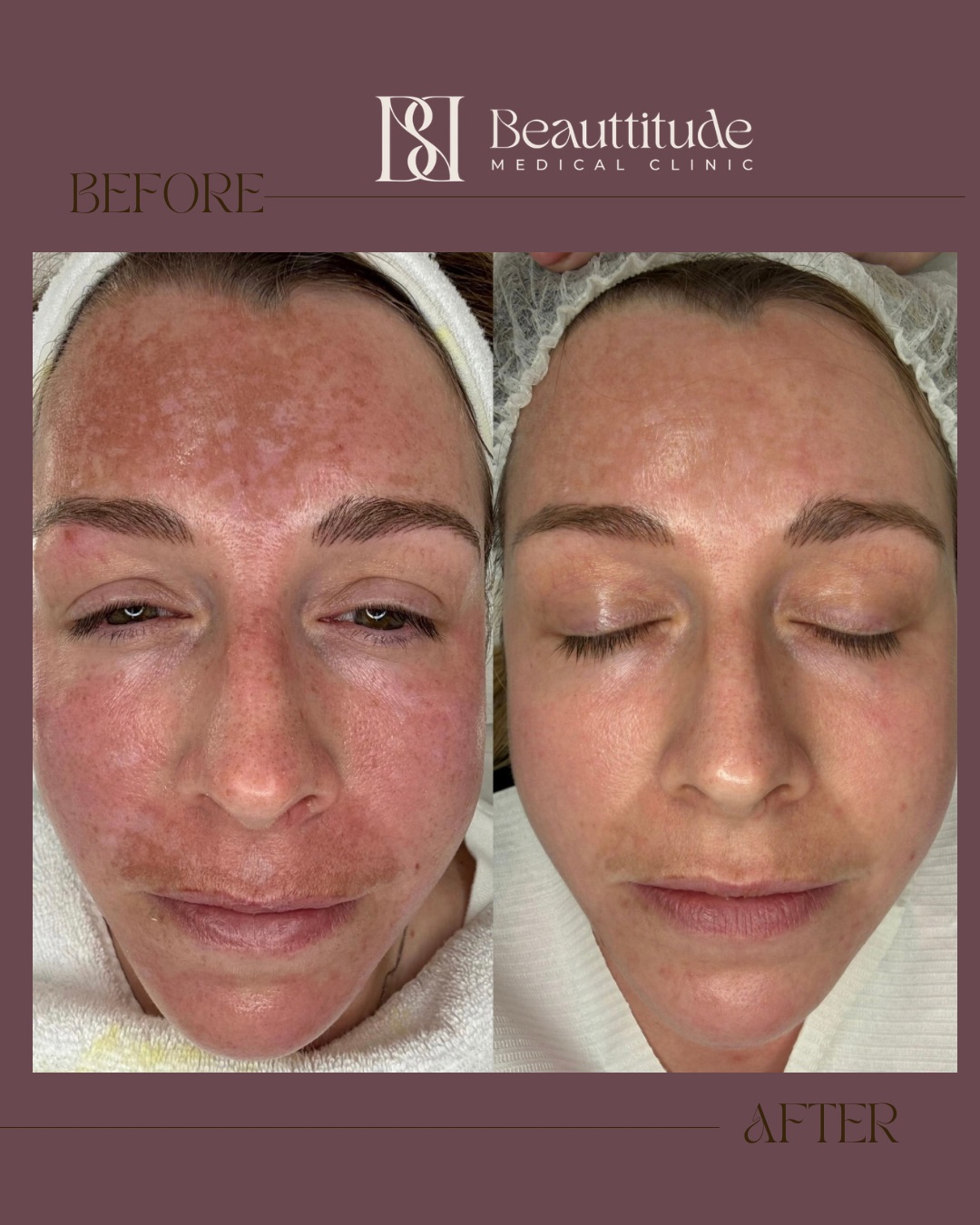
The first time I saw these photos, I knew this was not going to be a straightforward case. Severe melasma. Deep, diffuse pigmentation spread across both cheeks , perioral and the forehead. The kind of presentation that a lot of patients have already spent years and significant money trying to address, with little to show …
The first time I saw these photos, I knew this was not going to be a straightforward case.
Severe melasma. Deep, diffuse pigmentation spread across both cheeks , perioral and the forehead. The kind of presentation that a lot of patients have already spent years and significant money trying to address, with little to show for it. The kind that requires not just the right protocol, but the right mindset , from both the patient and the doctor.
What followed was six months of consistent work, honest conversations, difficult weeks, and a result that still makes me pause when I look at it. I’m sharing it because I think it tells a story that matters , not just about what is possible with the right treatment, but about what it actually takes to get there.
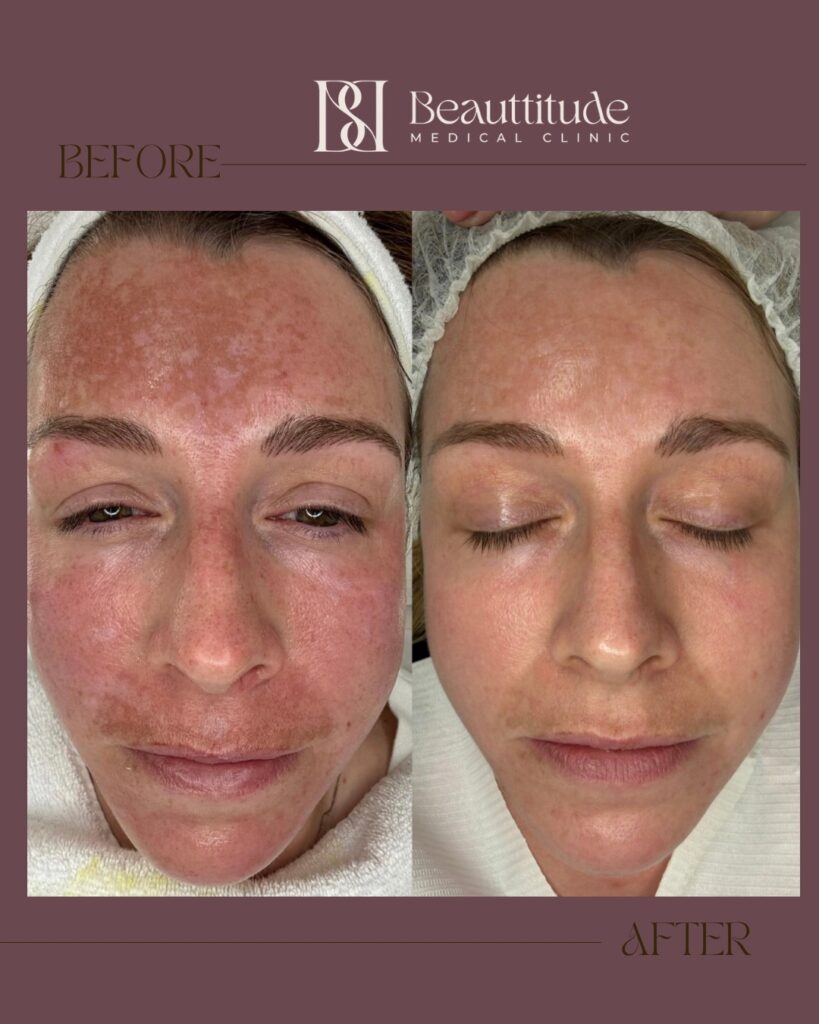
6 months.
Obagi Nu Derm protocol.
This is what consistency and the right guidance looks like. Training your skin to let go of what it has been holding onto is some of the most patient, most rewarding work there is. And you don’t have to do it alone.
Dr Gabriela
Beauttitude Medical Clinic
What melasma actually is and why it’s so hard to treat?
Melasma is a chronic pigmentation condition driven by an overproduction of melanin , the pigment that gives skin its colour. It typically appears as symmetrical patches of brown or grey-brown discolouration across the cheeks, forehead, upper lip, and bridge of the nose.
The triggers are well established: UV exposure, hormonal fluctuations (pregnancy, contraceptive pill, HRT), heat, and inflammation. What makes it particularly challenging is that melanocytes , the cells responsible for producing melanin , become hyperactive and hypersensitive. Even small amounts of sun exposure or heat can reactivate pigmentation that seemed to be clearing.
Melasma also sits at different depths in the skin. Epidermal melasma affects the surface layers and tends to respond better to treatment. Dermal melasma sits deeper, is harder to reach, and takes considerably longer to shift. Mixed-type melasma , which is what many patients with severe presentations have , involves both layers simultaneously, which is what makes it one of the most complex pigmentation conditions to manage.
This patient had mixed-type melasma with a significant dermal component. That context matters, because it explains both the protocol I chose and the timeline I was honest with her about from the very first consultation.
Why I chose the Obagi Nu Derm protocol?
The Obagi Nu Derm System is a doctor-prescribed skincare protocol designed to work at a cellular level — addressing pigmentation, skin texture, and overall skin health simultaneously. It combines prescription-strength tretinoin (a retinoid that accelerates cell turnover) with hydroquinone (a melanin-suppressing agent), alongside supporting products that prepare the skin, manage sensitivity, and protect the results.
It is not a gentle system. It is not designed to be. The philosophy behind Obagi Nu Derm is that in order to fundamentally retrain how the skin behaves, you need to work at a depth that most over-the-counter products simply cannot reach. That requires prescription-grade ingredients, consistent use, and — crucially — medical supervision throughout.
For a case like this one, with deep, stubborn, hormonally driven melasma, it was the most clinically appropriate choice available.
The part nobody tells you about: months one to three
This is the part of the blog I most want people to read.
The first two to three months on the Obagi Nu Derm protocol are hard. Not emotionally hard in the way you might expect from a confidence journey , hard in the sense that your skin will look worse before it looks better. This is not a side effect. It is the mechanism.
Tretinoin accelerates cell turnover at a rate the skin is not used to. The result is visible purging: skin that flakes, peels, becomes dry and sensitive, and in many cases looks more congested or more pigmented in the early weeks as deeper layers are brought to the surface. For a patient already dealing with difficult skin, this phase can feel devastating.
My patient messaged me during those months. More than once. The questions were always a version of the same thing: is this normal? Should I stop? Is it getting worse?
The answer every time was: this is exactly what is supposed to happen. Stay the course. And she did.
I want to be clear about something: without that consistent contact, without someone on the other end confirming that the process was working even when it didn’t look like it, I believe most patients would have stopped. Not because they lacked commitment, but because there is no visible reward in those early weeks to keep you going. The guidance is the reward. The guidance is what makes the difference between a treatment that works and a product that gets abandoned.
Managing this case at a distance
This patient doesn’t live in the same city as the clinic. Every consultation happened online.
I want to address that directly, because I think there is still a perception that meaningful aesthetic medicine requires the patient to be physically present at every stage. For certain treatments, that’s true. For a protocol-based skincare journey like this one, consistent online follow-up , with good photography, honest communication, and the ability to adjust in real time — works.
What it requires is structure. We had a clear check-in schedule. Photos at every online appointment, same lighting, same angles. Questions answered promptly. Adjustments made to the protocol when needed. And a patient who showed up to follow-up online , even when her skin was at its most difficult.
What it also required was collaboration.
The collaboration that completed the picture
One of the things I’m most proud of in this case is that I didn’t try to manage it entirely alone.
Because my patient was based remotely, I reached out to a trusted skin therapist clinic in her area , someone whose clinical judgement I had confidence in , and we worked together. She carried out two sessions of professionally applied chemical peels, timed strategically around the Nu Derm protocol to enhance penetration and accelerate the pigmentation shift. She also delivered one session of Spongilla Fusion treatment, which uses bio-microneedling to create micro-channels in the skin that significantly boost the absorption of active ingredients applied immediately after.
The combination of the home protocol and these in-clinic sessions, coordinated across distance, is what gave the result its depth. Neither element alone would have achieved this.
Melasma is not untreatable. But it requires the right approach, realistic expectations, and consistent support.
The most important thing I can tell you is this: if you have tried products, tried treatments, and felt like nothing is working , the missing piece is almost always the guidance. Not a better product. A better relationship with someone who understands your skin, can explain what is happening at every stage, and can keep you going when the process feels invisible.
That is what I do at Beauttitude Medical Clinic. Whether you are local or on the other side of the country or outside UK, I offer thorough skin consultations, in person and online , where I look at your skin concerns understand its cause and depth, and build a treatment plan that is honest about what it takes.
Your skin is worth that kind of investment. And you deserve a doctor who will stay in it with you for the whole journey.